Hi Francois,
Thank you for sharing CNESM’s analysis of the ATR pilot and relevance to Quebec context for practice.
Your team’s point that ATR is a reasonable assessment scale to think of transition from both ACT and ICM, but not in identifying where a client’s fit in form of service between them is a critical point of focus on it’s usefulness to system care planning.
When I think about our context here in Ottawa, with the team I work with “Step-down from ACTT” there is a marked difference overall in team contrasts…overall. But for sure there is not a full distinction between client program caseloads. Even with the ATR’s cut off scores, the approach to the pilot with teams, as with Gary Cuddeback’s ATR manual, emphasizes the assessment as one of the benchmarks/guide for teams to think about transition, shift in service.
For me, as a “champion” of the scale a key motivator for doing this, was drawing from perspectives from New York state, where their administrative assessment of service fit, was somewhat mechanical in its identification of clients needing to move on from ACTT. An innovation from one NY team that came out of this was the development of a recovery and medication scale (beta) https://www.eenetconnect.ca/top...on-client-transition .
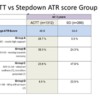
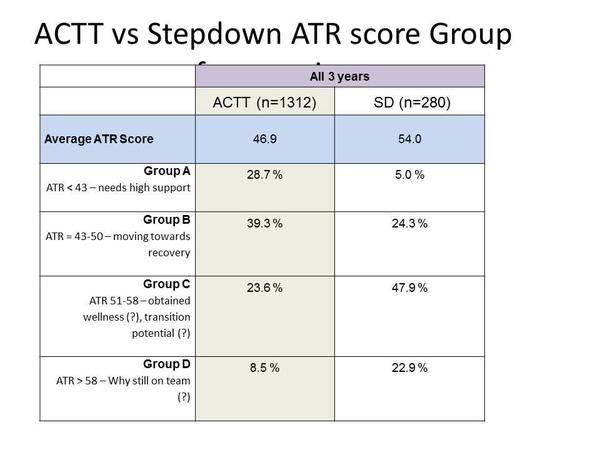
So again, while differences, not distinctive, as below. Though it should be noted, for our Step Down from ACTT team context, we are a form of ICM with the pretty well unique context of being: interdisciplinary with a psychiatrist. It would be interesting to learn from other forms of service, post ACT that are being initiated in Ontario.
By the way, just to step back…in time and look at the challenges in differences between ACT vs. ICM, I found the point made by Robert King http://escholarship.umassmed.e...1036&context=pib that in the mental health system evaluation, ACT’s stand alone “gold standard” of evidence base, has been a leading edge for system development of ICM, for example Ontario’s evidence for ICM standard of care are founded on ACT evidence informed components.
I think teams in Ontario, would benefit from hearing about your use of the Colorado, because of the approach that CNESM used in implementing it and your efforts at encouraging fidelity to the ACT model – and good practice, IE: emphasis on supervision, form of ensuring team focus on recovery planning with clients.
So, I am just sharing a comment to you as a front line worker, who has been focused on transition practices. I realize many factors in play for all of us, but I look forward to further exchange.